Unlocking the Vital Role of Estradiol in Male Sexual Health: Looking Beyond Testosterone
Exploring the Complex Interplay of Estradiol and Androgens in Male Sexual Health
Beyond the Shadows of Testosterone
Originally published on March 3rd, 2017. Updated on October 30th, 2023.
In the intricate realm of male urological health, the pivotal role of estradiol in male sexual well-being often remains in the shadows of its androgenic counterpart, testosterone. To achieve a comprehensive understanding, we must recognize the profound significance of estrogens, particularly estradiol. This article elucidates the importance of maintaining a delicate hormonal equilibrium, highlighting that neither hormone inherently outshines the other. Optimal health hinges upon the harmonious interplay of these fundamental actors.
What is Estradiol?
The Quintessential Estrogen
Estradiol, colloquially referred to as E2, stands as the most potent manifestation among the estrogens—a group of hormones primarily associated with female physiology. While its influence on the female reproductive system and secondary sexual characteristics garners recognition, estradiol's presence within the male body warrants equal acknowledgment. Originating predominantly from the male testes, it orchestrates a multitude of physiological processes. These encompass influences on libido, erectile function, and even the intricate choreography of spermatogenesis—culminating in the formation and maturation of sperm cells.
Hormonal Dynamics and Estradiol's Crucial Impact
From Testosterone to Estradiol: The Aromatization Pathway
Testosterone, the primary male sex hormone, does not operate in isolation but undergoes a transformative process known as aromatization. Through this process, testosterone metamorphoses into estrogen variants: estrone and estradiol. The orchestration of this pivotal conversion is executed by the aromatase enzyme present in various tissues, including adipose tissue and the brain. While estradiol's role in the female reproductive cycle is well-established, its equally fundamental role in counterbalancing testosterone's effects within the male body is often overlooked. This intricate interplay of hormones is essential for maintaining overall health.
The Scientific Landscape of Estradiol
Estradiol in Men: The Uncharted Territory
Historically, estradiol's significance in men has remained underexplored. As our understanding expands, we gain insights into the intricacies of its synthesis, particularly the role of the enzyme 17β-hydroxysteroid dehydrogenase. This enzyme orchestrates the conversion of testosterone into estradiol. Contrary to conventional viewpoints that often position testosterone as the linchpin of male sexuality, modern research shines a spotlight on estradiol as an equal collaborator, moderating myriad facets of male sexual function.
The Neurological Nexus of Estradiol and Libido
Decoding the Brain-Hormone Connection
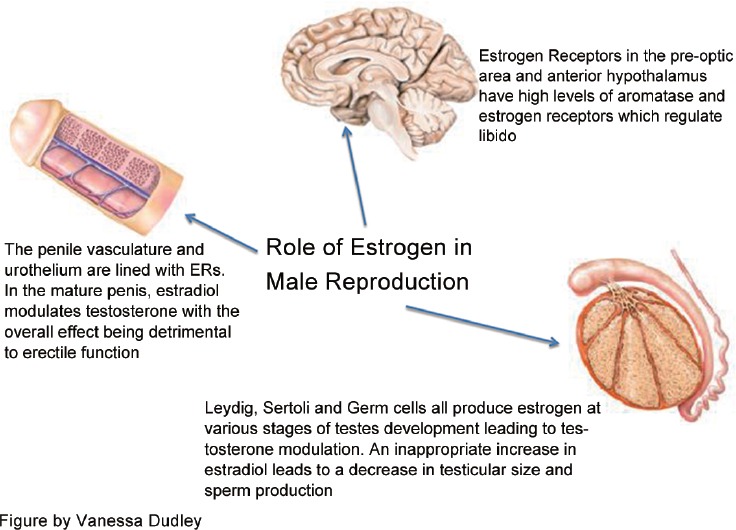
Estradiol's sphere of influence transcends mere hormone-to-hormone interactions; it deeply intertwines with the neuroendocrine system. By binding to estrogen receptors (ER) and engaging with aromatase receptors in the brain, estradiol navigates pathways fundamental to arousal and libido. The abundance of these receptors in the pre-optic area and hypothalamus underscores the centrality of the brain's rapport with estradiol in comprehending the full panorama of male sexual health.

The Dual Nature of Estradiol: The Enigma of Low Testosterone
Surprising Findings in Cases of Low Testosterone
Instances of low testosterone unveil intriguing facets of estradiol. In scenarios where testosterone levels plummet, exogenous supplementation of estradiol has demonstrated the capacity to counteract diminished libido. This phenomenon hints at the neuroprotective attributes of estradiol, particularly evident in treatments like androgen deprivation therapy (ADT) for prostate conditions. In such contexts, the pivotal role of estradiol takes center stage, especially when testosterone's reliability proves insufficient.
Unveiling the Complexity: Estradiol and Healthy Testosterone
A Balancing Act in the Male Hormonal Landscape
When considering men with standard testosterone levels, the discourse becomes more nuanced. While one study reported a decline in facets like "sexual interest, fantasy, masturbation, and erections" due to supplemental estradiol, another indicated different results. This divergence accentuates the need for a nuanced perspective on estradiol's impact across varying hormonal backgrounds.
Navigating Male Sexual Health: A Holistic Perspective
What Does Clomiphene Citrate Teach Us About Libido?
Clomiphene citrate, commonly known as Clomid, imparts distinctive insights when addressing male sexual health. Recognized predominantly for its role in treating female infertility, Clomid, in men, assumes the task of elevating testosterone levels. Nonetheless, a captivating observation arises wherein despite this elevation, numerous men convey that their symptoms of low testosterone remain unaffected by Clomid treatment, encompassing the persistence of subdued libido. This phenomenon underscores the notion that male libido and the overall sensation of vitality transcend the confines of testosterone levels alone. When Clomid interfaces with estrogen receptors, it triggers the hypothalamus to release hormones, thereby influencing the delicate equilibrium between testosterone and estradiol. This equilibrium, combined with the aforementioned observations, accentuates the fact that comprehending male libido and reproductive health mandates a deeper exploration beyond mere testosterone metrics.
The Influence of Estradiol on Erectile Function
From Developmental Phases to Adult Implications
Estradiol's role transcends the realm of libido. It profoundly molds erectile function through multifaceted mechanisms. During developmental stages, disproportionate exposure to estradiol can impede penile growth, potentially setting the stage for erectile challenges in adulthood. In mature phases, elevated estradiol disrupts blood vessel dynamics within the penis, occasionally precipitating conditions like venous leakage. Grasping the extent of estradiol's influence facilitates a comprehensive grasp of male sexual health.
A Multi-Faceted Role in Male Reproductive Dynamics
Diving Deep into Spermatogenesis and Reproductive Health
Estradiol doesn't confine its influence to libido and erections; it probes deeper into male reproductive health. Its presence orchestrates the modulation of spermatogenesis—an intricate process orchestrating sperm production and maturation. Appropriate levels of estradiol facilitate this process, yet any imbalance, especially an excess of estradiol, can perturb this intricate dance, exerting repercussions on male fertility.
Striking the Balance: Estradiol's Role in Male Sexual Health
Redefining "Good" and "Bad" in Hormonal Dynamics
The intricate choreography between androgens, such as testosterone, and estrogens, particularly estradiol, lays the cornerstone of male sexual health. Disregarding estradiol as a mere supporting cast undermines our comprehensive understanding. Grasping the significance of sustaining a balanced rapport between these hormones assumes paramount importance. In the pursuit of optimal male sexual health, the watchword remains equilibrium.
In Summary
The Harmonious Dance of Hormones
Male sexual health transcends the confines of testosterone alone. Estradiol, with its multifaceted roles, constitutes a substantial contributor. Recognizing its significance shatters conventional assumptions, necessitating a reappraisal of its role in libido, sexual performance, and fertility. To holistically apprehend male sexual health, it becomes imperative to perceive estradiol and testosterone not as adversaries but as collaborators orchestrating a harmonious performance.
Key Takeaways:
- Significance of Estradiol in Male Sexual Health: Estradiol, typically associated with female reproductive health, is pivotal in the intricate domain of male sexual well-being.
- Hormonal Balance: Ideal male sexual health depends on the nuanced balance between male sex hormones, like testosterone, and female sex hormones, such as estradiol.
- No Inherently "Good" or "Bad" Hormones: An oversimplified good/bad dichotomy for hormones fails to capture their intricate interplays. Both androgens and estrogens possess unique, essential roles, demanding a delicate balance for overall well-being.
- Neuroendocrine Nexus: Estradiol's sphere of influence expands beyond mere hormonal dynamics, delving deep into the sophisticated neuroendocrine system where neural receptors modulate libido.
- Benefits of Estradiol Supplementation in Cases of Low Testosterone: In instances of low testosterone, estradiol supplementation emerges as a potential remedy, enhancing libido and alleviating sexual health challenges.
- Balancing Testosterone Levels: For sustaining male sexual desire, performance, and reproductive health, maintaining a balanced level of estradiol and testosterone is crucial.
- Impact on Erectile Function: Estradiol's multifaceted role in erectile function ranges from early developmental stages to its effects on penile vasculature permeability.
- Influence on Sperm Production and Maturation: Estradiol's reach extends to male reproduction, affecting processes like sperm maturation and production in nuanced ways that demand equilibrium.
- Complex Interplay: The harmonious collaboration between androgens and estrogens governs male sexual health, highlighting the necessity to fathom estradiol's multifarious roles.
References:
Site Disclaimers
General Guidence
The content on this site is provided for educational and informational purposes only and should not be construed as medical advice. Always consult a qualified healthcare provider before making changes to your diet, lifestyle, or health regimen, particularly if you are pregnant or nursing, under the age of 18, managing allergies or known sensitivities, or living with any medical conditions.
At RAW Forest Foods, your safety is our priority. Please note that our products are dietary supplements, not medications. The following disclaimer applies:
* These statements have not been evaluated by the Food and Drug Administration. These products are not intended to diagnose, treat, cure, or prevent any disease.
Ingredient Transparency and Allergen Awareness
We are committed to providing transparent ingredient information to help you make informed decisions. If you have or suspect you have allergies to any of our ingredients, we strongly advise against using our products, as allergic reactions can be severe.
Interaction with Medications
If you are taking any medications, consult with your healthcare provider before using supplements. Certain supplements may interact with medications, potentially altering their effectiveness or causing unwanted effects.
For more details, please review our full Terms and Conditions.