Vitamin D, SHBG, and Testosterone
The Importance of Vitamin D
Vitamin D is a fat-soluble vitamin, technically a secosteroid—a type of steroid. Many biological processes within the body rely on vitamin D, though its major functions are regulating the absorption of calcium, iron, magnesium, phosphate, and zinc in the small intestine, and promoting healthy growth and bone remodeling. It is because it plays such a major role in calcium regulation that a lack of vitamin D can lead to osteomalacia or rickets. Without adequate levels of vitamin D, the body can only absorb roughly 10-15% of dietary calcium, compared to 30-40% absorption with adequate vitamin D levels.
Beyond calcium and bones, vitamin D receptors are present throughout the body, including in the blood vessels, endocrine glands, heart, muscles, prostate, and the small intestine. For the sake of this article, it is the “other” functions of vitamin D that are the most relevant.

The Sunshine Vitamin or the Sunshine Hormone?
Vitamin D is the sunshine vitamin. Unlike other vitamins, vitamin D is largely absent in foods, yet it is an essential vitamin for health. Under ideal circumstances, the body synthesizes vitamin D on its own. Using cholesterol ( 7-dehydrocholesterol), present in the skin, sunlight (specifically UVB energy) converts cholesterol into vitamin D3 (otherwise known as cholecalciferol), where it then travels to the liver and then to the kidneys, where enzymatic conversion (hydroxylation) takes the inactive D3 and turns it into the active form.
At the liver, additional oxygen and hydrogen molecules are attached to vitamin D3 (cholecalciferol) to convert it into 25-hydroxyvitamin D, also known as 25(OH)D. From the liver, 25(OH)D travels to the kidneys, where it picks up an additional pair of oxygen and hydrogen molecules, whereby it is converted to its final and active form of vitamin D: 1,25 dihydroxyvitamin D, known commonly as calcitriol and abbreviated as 1,25(OH)2D. Generically, all of these forms are commonly referred to as vitamin D (Harvard School of Public Health).
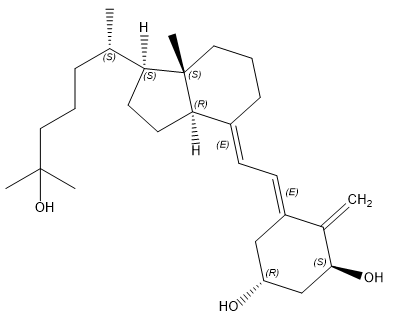
When testing for vitamin D levels, 25-hydroxyvitamin D, also known as 25(OH)D, is measured (as produced in the liver).
Healthy Vitamin D Levels
In 2010, the Institute of Medicine (IOM) recommended in the Dietary Reference Intakes for Calcium and Vitamin D publication a blood level of 20 ng/mL for the prevention of bone-related disease. However, in 2011, the Endocrine Society published a report stating that, at a minimum, vitamin D levels should be at 30 ng/mL. But that, because of issues with the accuracy of tests, levels should be between 40 and 60 ng/mL. Note that the lower recommendation was in relation to bone health and that the higher recommendation was published by the highly respected Endocrine Society.
Yet others recommend even higher levels of the vitamin. Dr. Christiane Northrup recommends vitamin D levels at between 50 and 100 ng/mL, but others consider anything above 60 ng/mL to be problematic.
The recommendations of the Endocrine Society that vitamin D levels should be between 40 and 60 ng/mL seem both adequate and safe.
Vitamin D Deficiencies
As life continues to move indoors (as opposed to working outside in the sunlight), synthesizing enough vitamin D becomes problematic. Additionally, in the northern hemisphere, anyone north of the 37-degree latitude line (in the US from San Francisco to Philadelphia and in Europe anything north of Sicily) will not be able to synthesize enough vitamin D in the winter. The use of sunscreen impairs the body’s ability to synthesize vitamin D since it blocks UVB rays, and obesity also decreases synthesis.
Vitamin D deficiency can lead to a myriad of symptoms, illnesses, and diseases, including:
- Depression;
- Increased risk of falls and fractures (most notably in the elderly population);
- Light-headedness;
- Muscle aches and weakness;
- Muscle twitching;
- Osteomalacia / rickets;
- Osteoporosis;
- Periodontitis;
- The proliferation of several cancers, including breast, colon, ovarian, and prostate cancer.
Vitamin D and Testosterone
There is a direct correlation between levels of vitamin D, 25(OH)D, and testosterone. Most likely, vitamin D has some type of regulatory effect on the hypothalamus-pituitary-testicular axis, owing to the presence of vitamin D receptors throughout it. Study after study has demonstrated the importance of adequate vitamin D levels in maintaining healthy, high levels of testosterone. Here are several references available for further research and citation:
- Additive benefit of higher testosterone levels and vitamin D plus calcium supplementation in regard to fall risk reduction among older men and women.
- Association between plasma 25-OH vitamin D and testosterone levels in men.
- Association of vitamin D status with serum androgen levels in men.
- Effect of vitamin D supplementation on testosterone levels in men.
- Influence of ultraviolet irradiation upon excretion of sex hormones in the male.
- Vitamin D is significantly associated with total testosterone and sex hormone-binding globulin in Malaysian men.
Additionally, at least in animal models, vitamin D and sperm quality and number are linked:
- Effect of vitamin D repletion on testicular function in vitamin D-deficient rats.
- Vitamin D is necessary for reproductive functions of the male rat.
- Vitamin D is positively associated with sperm motility and increases intracellular calcium in human spermatozoa.
As stated above, vitamin D receptors are found throughout the hypothalamus-pituitary-testicular axis, and vitamin D influences hypogonadism (low to no testosterone production in the testes).
- Association of hypogonadism with vitamin D status: the European Male Ageing Study.
- Hip fracture in elderly men: the importance of subclinical vitamin D deficiency and hypogonadism.
- Is there a role for vitamin D in human reproduction?
In summation, vitamin D levels and testosterone levels are linked; vitamin D influences the functioning of the hypothalamus-pituitary-testicular axis, and hypogonadism (low testosterone production in the testes) is associated with vitamin D levels. Additionally, at least in animal models, vitamin D is necessary for proper sperm production.
Vitamin D and Sex Hormone Binding Globulin (SHBG)
Sex hormone binding globulin (SHBG) is a glycoprotein present in the blood that binds to both testosterone and estrogen (though it has a greater affinity for testosterone). Free testosterone, also known as active testosterone, is the portion of the overall testosterone present that is not bound to SHBG. It is only the unbound (active, free) testosterone that can enter a cell and activate a testosterone receptor. The higher the level of SHBG, the lower the amount of free, unbound, active testosterone.
High levels of estrogen (estradiol) cause an increase in sex hormone binding globulin, as do high levels of thyroxine (the thyroid prohormone T4). High levels of androgens, growth hormone, insulin-like growth factor 1 (IGF-1), insulin, prolactin, and transcortin cause a decrease in SHBG (which for most is the goal—although clinically low levels are undesirable, increasing the probability of type 2 diabetes). As noted elsewhere, Nettle Root (Urtica dioica Radix) is able to bind and thus “deactivate” SHBG.
Vitamin D lowers sex hormone binding globulin, although the exact method of action is unclear. Several studies showed a significant impact on vitamin D levels and levels of SHBG ( 1, 2, 3).
In one study, Association of Vitamin D Status with Serum Androgen Levels in Men, researchers noted that:
Men with sufficient 25(OH)D levels (≥30 μg/l) had significantly higher levels of testosterone and FAI and significantly lower levels of SHBG when compared to 25(OH)D insufficient (20–29 μg/l) and 25(OH)D-deficient (<20 μg/l) men (P < 0.05 for all).
RDA and Food Sources of Vitamin D
The current USDA recommended daily allowance for vitamin D is 600 IU for men and women from ages 18-70 ( USDA, Mayo Clinic). However, complications arise in elevating low vitamin D levels, as there is a yet-to-be understood nonlinear relationship between vitamin D supplementation and an increase in serum vitamin D levels.
The recommended daily allowance (RDA) is for maintenance of vitamin D, not for increasing low levels. Furthermore, the aforementioned publication of the Endocrine Society states a daily recommended intake of 1500-2000 IU—considerably more than the RDA—for healthy vitamin D levels. To learn more about supplementation strategies for increasing established low vitamin D levels, please see our article Repairing Low Vitamin D.
Food Sources of Vitamin D |
||
|---|---|---|
| Food Sources | Level of Vitamin D (IU) | Daily Value (%) |
| Cod liver oil, 1 tablespoon | 1,360 | 340 |
| Swordfish, cooked, 3 ounces | 566 | 142 |
| Salmon (sockeye), cooked, 3 ounces | 447 | 112 |
| Tuna fish, canned in water, drained, 3 ounces | 154 | 39 |
| Orange juice fortified with vitamin D, 1 cup (check product labels, as the amount of added vitamin D varies) | 137 | 34 |
| Milk, nonfat, reduced fat, and whole, vitamin D-fortified, 1 cup | 115-124 | 29-31 |
| Yogurt, fortified with 20% of the DV for vitamin D, 6 ounces (more heavily fortified yogurts provide more of the DV) | 80 | 20 |
| Margarine, fortified, 1 tablespoon | 60 | 15 |
| Sardines, canned in oil, drained, 2 sardines | 46 | 12 |
| Liver, beef, cooked, 3 ounces | 42 | 11 |
| Egg, 1 large (vitamin D is found in yolk) | 41 | 10 |
| Ready-to-eat cereal, fortified with 10% of the DV for vitamin D, 0.75-1 cup (more heavily fortified cereals might provide more of the DV) | 40 | 10 |
| Cheese, Swiss, 1 ounce | 6 | 2 |
| Source: USDA | ||
The Take Home Message on Vitamin D and Androgenic Hormone Health
The take-home here is not simply that vitamin D and testosterone, hypogonadism, sperm production, and SHBG are linked. They are, and having your vitamin D levels tested is important, especially if you live in a northerly or southerly geographic area, or if you are experiencing low testosterone or high SHBG. But also highlighted here is the overall complexity of the endocrine system and how seemingly unrelated processes within the body regulate and influence others.
Site Disclaimers
General Guidence
The content on this site is provided for educational and informational purposes only and should not be construed as medical advice. Always consult a qualified healthcare provider before making changes to your diet, lifestyle, or health regimen, particularly if you are pregnant or nursing, under the age of 18, managing allergies or known sensitivities, or living with any medical conditions.
At RAW Forest Foods, your safety is our priority. Please note that our products are dietary supplements, not medications. The following disclaimer applies:
* These statements have not been evaluated by the Food and Drug Administration. These products are not intended to diagnose, treat, cure, or prevent any disease.
Ingredient Transparency and Allergen Awareness
We are committed to providing transparent ingredient information to help you make informed decisions. If you have or suspect you have allergies to any of our ingredients, we strongly advise against using our products, as allergic reactions can be severe.
Interaction with Medications
If you are taking any medications, consult with your healthcare provider before using supplements. Certain supplements may interact with medications, potentially altering their effectiveness or causing unwanted effects.
For more details, please review our full Terms and Conditions.






